Raising kids is tough. Raising children with food allergies is even tougher!
In the past, completely avoiding the food allergen or delaying the introduction of other allergenic foods was the focus of management. Now the management of food allergies is more proactive and targeted at improving a child’s dietary variation, quality of life and reducing food phobias – but of course, within safe boundaries.
We’ll answer some common questions and concerns parents have about food allergies:
Who is affected by food allergies?
Food allergies affect approximately 4-5% of Singaporean children.
What foods trigger these allergies?
Cow’s milk, egg, peanut, tree nut, fish, soy and wheat allergy are the most common types of food allergies seen worldwide. The frequency differs from country to country.
Shellfish (prawns, crabs etc) are the most common allergenic food in Asian teenagers and adults.
How do food allergies occur?
Food allergies occur when the body’s immune system sees the food protein as a foreign invader and sends immune soldiers to attack it when it shouldn’t. There are 2 main groups of allergies:
For IgE-mediated allergic reactions, the immune soldiers are IgE antibodies. They attack a specific food protein leading to a fast onset of itchy rashes, hives and eye/lip/facial swelling. Each time the food protein is seen, the IgE antibody allergic attack can get stronger resulting in anaphylaxis. Anaphylaxis is when the allergic reaction causes life threatening symptoms such as airway swelling, breathlessness, or decreased blood circulation.
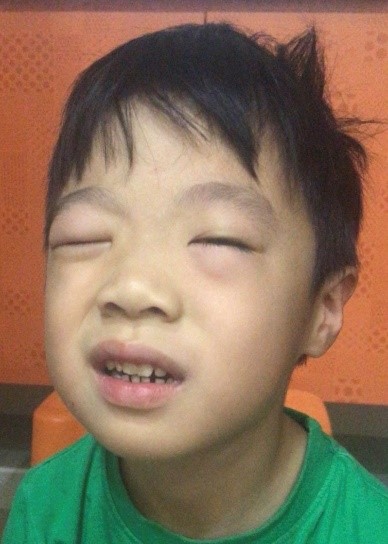
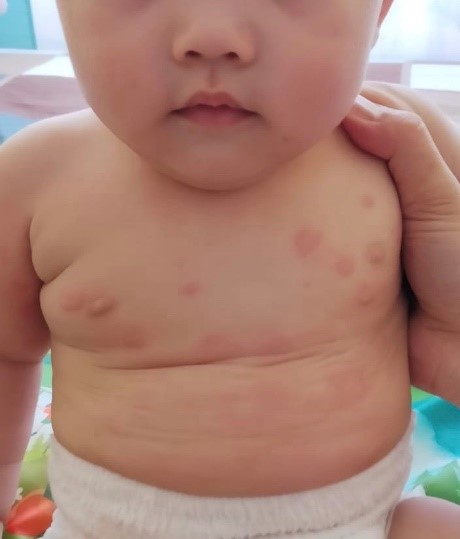
Non-IgE mediated allergies are much less common and more delayed in onset. There are several types of these allergies, but they typically result in significant vomiting or diarrhoea, and often blood-stained stools. Diagnosis can sometimes be difficult, hence if there is a suspicion of a food cause for vomiting or diarrhoea, one should consult a specialist.
Why is my child allergic?
Why some children get food allergies is not fully understood.
Eczema in a child or a family history of food allergy are risk factors food allergies. But this not always the case.
When do I need a doctor’s help?
When should you seek help? If your child has/had any of the following:
- An allergic reaction to food
- Significant eczema
- If you are not sure if your child has a food allergy
- If you are avoiding foods
A specialist will help confirm the diagnosis of a food allergy. Allergy testing (see below) are usually needed as well. We will teach you how to manage an allergic reaction, what foods to avoid and what foods to give.
For IgE mediated allergies, the following tests are usually done:
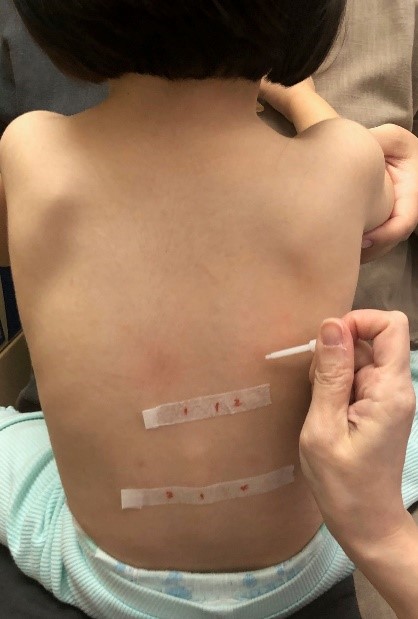
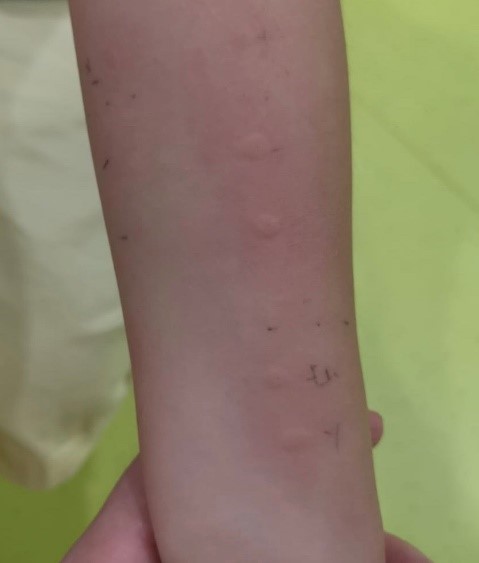
Skin Prick Test (SPT)
Skin prick testing is VERY safe, accurate and quick. It is usually not painful and there is no blood drawn. However, sometimes the child may be anxious and cry upon seeing the prick device. A child must stop taking antihistamines (e.g. runny nose and some cough medicines) for 5 days before doing this test. There is no age limit, but it can be less accurate in very young babies.
Allergy blood tests
Measuring specific levels of IgE to food proteins and the specific molecules on the protein in the blood can give more information about the severity of an allergy and a better indication as to whether it safe to do a food challenge.
Oral food Challenge (OFC)
The ultimate food allergy TEST is to give it to the child – this is called a food challenge! This is done, when the child has likely outgrown a food allergy; can likely take a safer form of the food protein (e.g. baked muffin in an egg allergic child) or when the food allergy is unlikely.
Because of the risks of an allergic reaction, it is usually done in a clinic/hospital. The food in question, is given in increasing amounts every 15-20 minutes in 4-5 steps. The child is closely monitored for any allergic reaction. When doing an OFC, a child should be totally well (not sick with fever, runny nose etc) and should not be on antihistamines for 5 days prior.
Treatments
Learning to manage an allergic reaction is vital for the safety of your child. Accidental ingestions of allergic foods will become more frequent especially as your child gets older.
Prevention of accidental ingestions is important. Learn to read ingredients of food labels and avoid eating in places where food labelling is poor and the chances of cross contamination high (e.g. food courts).
Oral antihistamines are used for mild reactions involving the skin only (e.g. hives, eye swelling).
For anaphylaxis (life-threatening allergic reaction), an injection with adrenaline is needed. An Epipen® (an injectable adrenaline pen) is provided to parents so they can save their own child, or sometimes an older child can save themselves before medical help arrives.
Food Oral Immunotherapy (OIT) has recently been started as a form of therapy in children with peanut allergy. While OIT is at the frontier of food allergy management, it requires commitment, and is high risk. Hence food OIT needs to be thoroughly discussed with a paediatric allergy specialist. There are research programs offering food OIT to other foods such as egg.

Paediatrician (Special Interest: Allergy & Immunology)
SBCC Baby & Child Clinic (Asthma, Lung, Sleep, Allergy & Paediatric Centre)
6 Napier Road #04-15 Gleneagles Medical Centre Singapore 258499









