
PULMONARY FUNCTION TESTS
Pulmonary or Lung function tests are an important component of lung assessment and provides objective information helpful for diagnosis, monitoring response to treatment and guide decisions regarding further treatment and intervention.
WHAT IS A PULMONARY FUNCTION TEST?
This is a test that determines how well the patient’s lungs and airways are working. The test helps the doctors to confirm diagnoses and follow the progress of a patient with lung disease e.g., asthma, and to assess the response to treatment. They measure things like:
• how much air you can take into your lungs
• how quickly you can blow air out of your lungs
• how well your lungs can take up oxygen
• the strength of your breathing muscles
• level of allergic inflammation in the airways
WHERE IS THE TEST PERFORMED?
The test is done in the SBCC Pulmonary Function Laboratory (Procedure Room), which is located at 6 Napier Road, Gleneagles Medical Centre, #04-01 Singapore 258499.
WHAT TYPE OF TESTS DO WE PERFORM?
▪ Spirometry (Baseline / with bronchodilator)
▪ Impulse Oscillometry (Baseline / with bronchodilator)
▪ Exhaled Nitric Oxide (FeNO)
▪ Lung Volumes
▪ Diffusing Capacity
▪ Exercise Challenge
▪ Maximal Respiratory Pressures
▪ Maximum Voluntary Ventilation
WHAT ARE ALL THESE TESTS ABOUT?
A) Spirometry (Baseline/with Bronchodilator)
▪ Spirometry can help to tell if your breathing is affected by narrowed or inflamed airways. The results are useful in diagnosing lung conditions, such as asthma. For some conditions, it can be used to grade how severe your condition is.
▪ Spirometry measures the amount of air you can breathe out from your lungs and how fast you can blow it out. You will be asked to take a very deep breath and blow out as fast as you can into a mouthpiece, until no more air comes out.
▪ A spirometry test typically takes 15 to 20 minutes, but it may be longer if it includes bronchodilator response testing. Bronchodilator responsiveness is done to see if your lung function gets better with medication, and if so, by how much. In bronchodilator responsiveness testing, the spirometry test is done before and after inhalation of airway medication typically Salbutamol MDI.
B) Impulse Oscillometry (Baseline/with Bronchodilator)
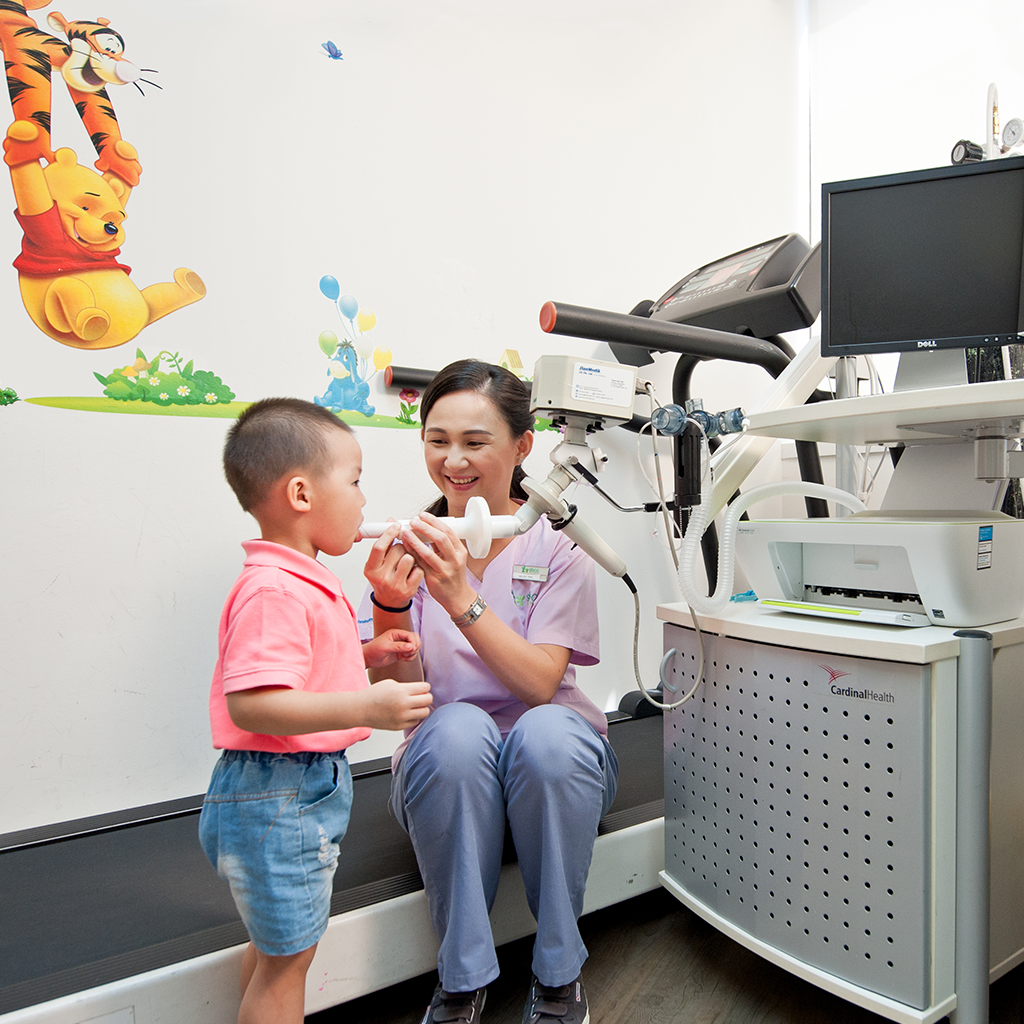
▪ Impulse Oscillometry (IOS) is a non-invasive, rapid, safe, and validated technique that measures respiratory impedance (resistance of the small and large airways, as well as the reactance of the airways) that is used as an indicator of lung function. It is a useful tool which helps in diagnosis and monitoring the progress of lung conditions.
▪ The technique of IOS is effort independent and it requires minimal patient cooperation. Hence, it is suitable for use in small children and frail adults.
▪ To perform IOS, the child is required to cradle his/her cheeks with their hands and hold a mouthpiece in place over a 30-second period while breathing normally (tidal breathing).
▪ IOS typically takes 10 minutes to complete, but it may be longer if it includes bronchodilator response testing. Bronchodilator responsiveness is done to see if your lung function gets better with medication, and if so, by how much. In bronchodilator responsiveness testing, IOS is done before and after inhalation of airway medication typically Salbutamol MDI.
C) Fractional Exhaled Nitric Oxide (FeNO)

▪ FeNO stands for fractional exhaled nitric oxide. It is found in the atmosphere and produced in the body, especially if there is inflammation.
▪ A fractional exhaled nitric oxide test is a simple test to see how much nitric oxide is in your breath. When you breathe out, your breath can show if you have inflamed airways. This test is useful to help your doctor understand if you have asthma. The measurements may also help your doctor determine if your current management plan is working properly and how your medication may need to be increased or reduced.
▪ To perform FeNO, you will be asked to breathe in deeply through a plastic mouthpiece/filter and then breathe out continuously (little by little until your lungs are empty) at a constant flow rate against a small resistance. The steady exhalation will normally take 10 seconds in older children and adults (6 seconds in younger children). Some devices will make a sound to help keep the flow at the right level throughout the test.
How Should I Prepare for a FeNO Test?
a) Avoid eating nitrate rich food, such as green leafy vegetables and beetroot a few hours before the test.
b) Avoid taking caffeine and alcohol 8 hours before the test.
c) No smoking of cigarettes at least 1 hour prior to test
D) Lung Volumes (Nitrogen Washout)
▪ A lung volume test is a way of measuring the total amount of air in your lungs, and how much air is left after you have breathed out as far as you can. This test helps the doctor to find out more about what is happening in your lungs. It can tell them if your lung condition is restrictive or obstructive.
▪ You will be asked to breathe in 100% oxygen and breathe out into a spirometer, with monitoring of nitrogen in the expired gas until all is washed out.
▪ The test can be completed in 10 minutes but may require longer than 15 minutes with severe airway disease.
E) Diffusing Capacity (DLCO)/Gas Transfer Test
▪ This test is used to measure how efficiently your lungs are working to take oxygen from the air you breathe in. It also tells your doctor how well your lungs can exchange oxygen from the lungs into the blood.
▪ You will be asked to take in a big breath through a mouthpiece while wearing a nose clip. You then hold your breath for a minimum of 10 seconds, then breathe out steadily into the machine. You will need to do this a few times, with a pause of 5 minutes in between to get reliable readings.
▪ The results will depend on the level of haemoglobin (Hb) in your blood and a Hb blood test will be done first prior to the test.
▪ The results can also be affected by smoking. Do not smoke for 24 hours before your test.
F) Exercise Challenge Test
▪ This test is used to determine if there is airway narrowing in relation to exercise.
▪ Your doctor may use this test to establish the diagnosis of Bronchial asthma or exercise-induced bronchoconstriction (EIB) which can also occur in patients without asthma.
▪ Before the exercising begins, you will need to undergo a baseline Spirometry/IOS assessment first. This step helps to ensure that it is safe to proceed with the exercise challenge test.
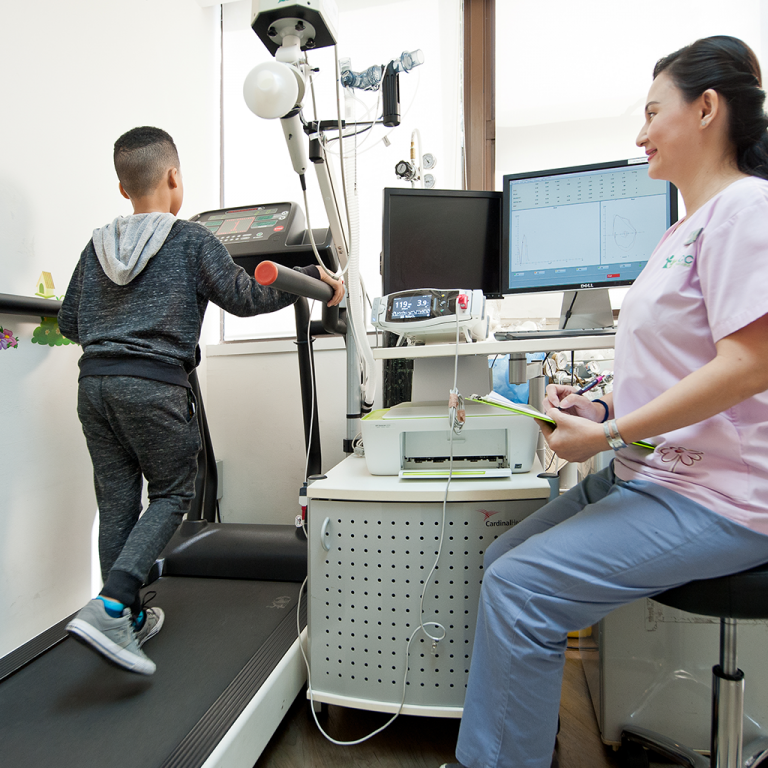
During the exercise, you will be asked to run on a treadmill at an incremental workload while your heart rate and oxygen are continuously monitored.
After the exercise is completed, you will repeat the lung function assessments at intervals of 3 minutes, 6 minutes, 10 minutes, and 15 minutes to detect any significant change in your lung function from the baseline readings.
At the end of post exercise Spirometry/IOS assessment, you may also be given an inhaled medication to re-open your airways if there is significant airway narrowing detected.
How Should I Prepare for Exercise Challenge Test?
a) Please come in comfortable clothing & footwear suitable for exercise and which do not restrict the breathing or movement of the chest.
b) Avoid taking short & long-acting bronchodilators/inhalers on the day of appointment or confirm with your doctor if there is any need to stop these medications.
– For short-acting bronchodilator (e.g., Ventolin), to stop at least 6 hours prior to test.
– For short acting muscarinic antagonist (e.g., Atrovent, Berodual), to stop at least 12 hours prior to test.
– For long-acting bronchodilator/combination inhaler (e.g., Symbicort, Seretide, Flutiform, Foster/Fostair) and Oral Theophylline (Nuelin SR) to stop at least 24 hours prior to test.
– For ultra-long-acting bronchodilator/combination inhaler (e.g., Breo or Relvar Ellipta) to stop at least 36 hours prior to test.
c) Avoid eating a heavy meal at least 2 hours prior to test.
d) No alcohol at least 8 hours prior to test
e) No smoking of cigarettes at least 1 hour prior to test
f) Do not carry out any strenuous activity 1 hour before the test
g) Please come in comfortable attire that do not restrict the movement of the chest
h) Do reschedule the appointment if you are feeling unwell on the day of the test
G) Maximal Voluntary Ventilation (MVV)
▪ This test is the measure of the neuromuscular and respiratory systems. It measures the respiratory muscle endurance and helps in evaluating respiratory muscle weakness.
▪ You will be asked to breathe in and out of a spirometer as fast and as deeply as possible for a duration of 12 seconds.
H) Maximal Respiratory Pressure (MIP & MEP)
▪ Maximal Respiratory Pressure test measures the strength of the muscles that help you breathe in and out. This can be assessed by measuring the maximal inspiratory pressure (MIP or PImax), and the maximal expiratory pressure (MEP or PEmax). The MIP reflects the strength of the diaphragm and other inspiratory muscles, while the MEP reflects the strength of the abdominal muscles and other expiratory muscles.
▪ There are two parts to the test –
Checking the strength of the muscles that help you breathe in:
– You will be asked to breathe out for as long as you can, and then suck hard on a mouthpiece for at least 1 second. It will feel like sucking a very thick milkshake through a straw. This is the maximal inspiratory pressure.
Checking the strength of the muscles that help you breathe out:
– You will be asked to breathe in deeply first and then blow out as hard as you can into a closed off mouthpiece. This is the maximal expiratory pressure.

Dr Jenny Tang
Paediatric (Asthma, Lung, Sleep & Allergy)
SBCC Baby & Child Clinic
Our Specialist
Dr Jenny Tang Poh Lin is a Paediatrician at SBCC Baby & Child Clinic with a special interest in Asthma, Lung, Sleep and Allergy. Prior to joining SBCC, Dr Tang held the position of Deputy Head of the Department of Paediatric Medicine, Head and Senior Consultant of the Respiratory Medicine Service and Medical Director of the Sleep Disorders Centre, KK Women’s and Children’s Hospital.
Common conditions managed by Dr Tang include asthma and lung disorders, sleep disorders, and allergy disorders.










